Radiofrequency (RF) Ablation can pinpoint spinal nerves that have been found to case chronic pain. A thin needle is placed in the center of the nerve, guided by ultrasound or a CT scanner and radiofrequency waves are used to vibrate or heat the nerve, killing only the part of the tissue causing pain and leaving the rest of the spinal nerve untouched.
The procedure may be performed under general anesthesia or conscious sedation. With conscious sedation, the patient receives pain medicine and sedation through an IV and skin-numbing medicine. Routine monitoring ensures patient safety during the procedure. Most patients feel little or no pain during the procedure and either go home the same day or the day after the procedure usually with no pain or soreness.
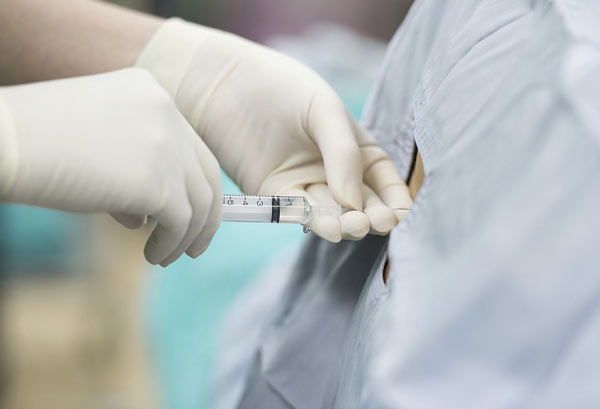
An Interventional Radiologist performs a spinal injection
Cryo Ablation is a process that uses extreme cold (cryo) to destroy or damage tissue (ablation). This procedure is used in a variety of clinical applications using hollow needles (cryoprobes) through which cooled, thermally conductive, fluids are circulated. Cryoprobes are inserted into or placed adjacent to tissue which is determined to be diseased in such a way that ablation will provide correction yielding benefit to the patient. When the probes are in place, the cryogenic freezing unit removes heat ("cools") from the tip of the probe and by extension from the surrounding tissues.
The most common application of cryoablation is to ablate solid tumors found in the lung, liver, breast, kidney and prostate. The use in prostate and renal cryoablation are the most common. Although sometimes applied through laparoscopic or open surgical approaches, most often cryoablation is performed percutaneously (through the skin and into the target tissue containing the tumor) by a medical specialist, such as an interventional radiologist.